[ad_1]
A 78-year-old man with progressive multiple sclerosis (MS) developed progressive multifocal leukoencephalopathy (PML) after treatment with ocrelizumab (Ocrevus) monotherapy. It is believed to be the first such case.
“Notably, the patient had never been treated with another disease-modifying therapy and did not carry any known predisposing diagnoses,” the authors say.
They note that other cases of PML have been diagnosed in patients after initiation of treatment with ocrelizumab; however, all of these cases were related to prior use of natalizumab (Tysabri) or fingolimod, and ocrelizumab had been deemed “noncontributory.”
“The take-home message from this case is that we need to gain more knowledge about the safety and efficacy of our immunotherapies in specific populations, such as elderly people with MS,” Asaff Harel, MD, Division of Neuro-Immunology, Lenox Hill Hospital, New York City, and Zucker School of Medicine at Hofstra/Northwell, Uniondale, New York, told Medscape Medical News.
Harel and colleagues describe the case in a report published online March 16 in JAMA Neurology.
Age Related?
At the time of presentation, the patient had been undergoing treatment with ocrelizumab monotherapy for 2 years. He presented with progressive visual disturbance and confusion of 2 weeks’ duration.
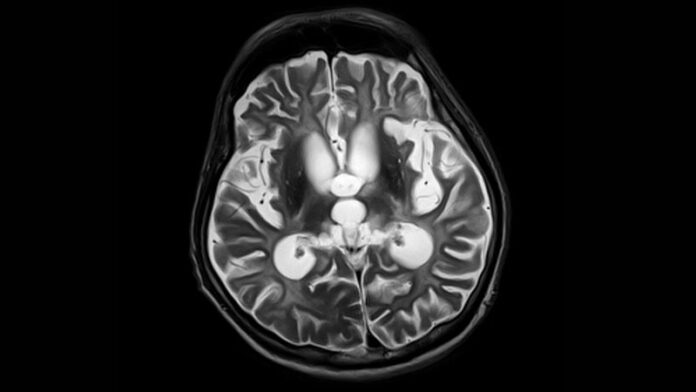
On examination, right homonymous hemianopia was noted. MRI showed an enlarging nonenhancing left parietal lesion without mass effect.
Testing of cerebrospinal fluid revealed JC virus, 1000 copies/mL, confirming the diagnosis of PML.
Blood work on diagnosis showed grade 2 lymphopenia. Results were as follows: absolute lymphocyte count, 710/μL; CD4, 294/μL (reference range, 325 – 1251 /μL); CD8, 85/μL (reference range, 90 – 775/μL); CD19, 1/μL; and preserved CD4/CD8 ratio (3.45). Serology was negative for HIV.
Retrospective absolute lymphocyte count showed intermittent grade 1 lymphopenia that preceded ocrelizumab treatment (absolute lymphocyte count range, 800 – 1200/μL).
The patient’s symptoms progressed over weeks to involve bilateral visual loss, right-sided facial droop, and dysphasia.
Ocrelizumab was stopped and off-label treatment with pembrolizumab (Keytruda) was initiated. The patient’s condition continued to decline rapidly, and he died 1 month after the initial PML diagnosis. Autopsy confirmed PML.
“While the precise mechanism that brings about PML is not entirely understood, it is likely facilitated by the decrease in lymphocyte production and potency associated with age-related immunosenescence,” Harel and colleagues write.
Although PML is rare with anti-CD20 therapy, this case “emphasizes the importance of a thorough discussion of the risks and benefits of ocrelizumab, especially in patients at higher risk for infections such as elderly patients,” they say.
Harel told Medscape Medical News that because both OPERA studies and the ORATORIO study of ocrelizumab recruited younger, ambulatory individuals, “we don’t have specific clinical trial data on the safety and efficacy of Ocrevus in patients who are elderly or wheelchair bound.
“Therefore, we have to think twice and use caution in extrapolating clinical trial efficacy and safety data to guide the care of such populations. In such populations, the risk/benefit equation may not be as clear-cut,” Harel said.
Harel has received personal fees from Teva Pharmaceuticals, Alexion Pharmaceuticals, Biogen, and Banner Life Sciences and grants from the National Multiple Sclerosis Society and Consortium of Multiple Sclerosis Centers.
JAMA Neurol. Published online March 16, 2021. Full text
For more Medscape Neurology news, join us on Facebook and Twitter.
[ad_2]
Source link