[ad_1]
Rheumatologists can look forward to the likely regulatory approval of the oral Janus kinase inhibitors tofacitinib and upadacitinib for the treatment of axial spondyloarthritis in the first half of 2021, speakers predicted at the 2021 Rheumatology Winter Clinical Symposium.
This will be a major advance in the treatment of axial spondyloarthritis (axSpA) and promises to be one of the overall highlights of the coming year in rheumatology, according to the speakers. Both medications are now under Food and Drug Administration review for the proposed new indication.
“My sense is within the next 6 months we’re going to have two different oral JAK inhibitors that offer a new option for our ankylosing spondylitis and axial spondyloarthritis patients,” predicted Eric M. Ruderman, MD, professor of medicine (rheumatology) at Northwestern University, Chicago.
Alexis R. Ogdie, MD, MSCE, noted that, at present, only two classes of potent medications are available for treatment of axial spondyloarthritis: tumor necrosis factor (TNF) inhibitors and anti–interleukin-17 biologics.
“I think it would be so exciting to have more treatment options. To have only two classes of drugs you can use for this disease is not enough,” said Ogdie, a rheumatologist and epidemiologist at the University of Pennsylvania, Philadelphia.
She and her fellow panelists also highlighted other recent key developments in axSpA, including epidemiologic evidence that case numbers are climbing sharply, identification of two previously unrecognized common comorbidities, a successful biologic remission induction and maintenance dose–reduction strategy, data on the best and worst biologics for patients with anterior uveitis, and evidence regarding next-step therapy in axSpA patients who’ve had an inadequate response to a TNF inhibitor.
Table of Contents
The JAK Inhibitors Are Coming
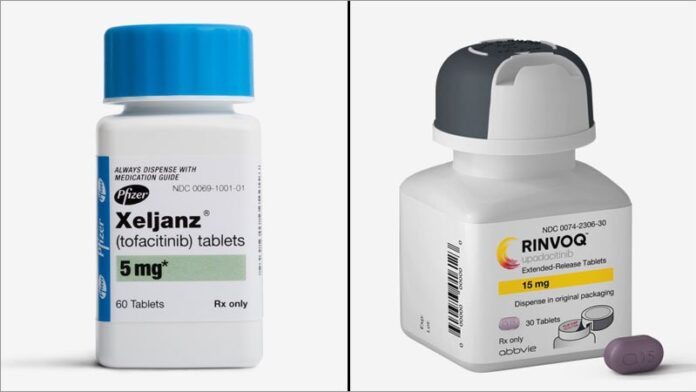
Oral tofacitinib (Xeljanz) at 5 mg twice daily was the focus of a pivotal phase 3, double-blind, 16-week, placebo-controlled clinical trial including 269 patients with axSpA. The results were presented at the 2020 annual meeting of the American College of Rheumatology. The primary endpoint was at least a 20% improvement in Assessment of Spondyloarthritis International Society response criteria (ASAS 20). This was accomplished in 56.4% of patients on tofacitinib and 29.4% of placebo-treated controls. The ASAS 40 response rate was even more impressive: 40.6% with the JAK inhibitor, compared with 12.5% with placebo. There was one serious infection in the tofacitinib group, but no cases of venous thromboembolism, interstitial lung disease, opportunistic infection, major adverse cardiovascular events, or malignancy in this brief 4-month study.
Also now under FDA review are data from SELECT-AXIS 1, a phase 2/3, double-blind trial in which 187 biologic-naive patients with ankylosing spondylitis were randomized to 14 weeks of upadacitinib (Rinvoq) at 15 mg once daily or placebo. The primary endpoint, an ASAS 40 response, occurred in 51.6% of patients on the JAK inhibitor and half as many controls.
“They saw improvement in MRI scores with upadacitinib, so there’s biologic plausibility to this,” Ruderman noted.
He predicted the JAK inhibitors are going to have a big impact in clinical practice, especially in men.
“I have a lot of ankylosing spondylitis and axial spondyloarthritis patients on NSAIDs who I’m not convinced are doing as well as they could, but they push back every time I raise the possibility of going on a biologic,” the rheumatologist said. “I suspect that, given the rapid response with JAK inhibitors here, as in rheumatoid arthritis, it might be a little bit easier to persuade these people to give this a try for 4-6 weeks and then see how much better they are. It’s a pill. You don’t have to give yourself a shot.”
Ogdie predicted the new oral agents will bring more axSpA patients into rheumatologists’ offices.
“I think it’ll be kind of like the apremilast effect in psoriasis, where the drug got a lot more people into the market,” she said.
U.S. Ankylosing Spondylitis Prevalence Rising
The diagnostic prevalence of axSpA in the United States increased by 86% between 2006 and 2014 in a retrospective analysis based on Medicare fee-for-service claims data. A separate analysis using IBM MarketScan data for the same years was confirmatory, showing a 56% increase, Jeffrey R. Curtis, MD, MS, MPH, of the University of Alabama at Birmingham reported at the 2020 annual meeting of the European League Against Rheumatism (EULAR), now known as the European Alliance of Associations for Rheumatology.
“I think the take home is we’re seeing more of this. Some of this is likely due to increased awareness and inclusion of nonradiographic disease,” according to Ruderman.
Two Previously Overlooked Comorbidities
It’s well recognized that 5%-10% of patients with axSpA have concurrent inflammatory bowel disease. But how about irritable bowel syndrome (IBS)?
A study of 186 Swedish patients with axSpA in the population-based SPARTAKUS registry, none with inflammatory bowel disease, concluded that 30% of them met ROME III diagnostic criteria for IBS, compared with 16% of healthy controls. Of note, the axSpA patients with comorbid IBS had significantly worse axSpA disease outcomes, compared with those without IBS as measured by pain, fatigue, and quality-of-life scores, as well as significantly greater disease activity on the Bath Ankylosing Spondylitis Disease Activity Index.
New-onset inflammatory back pain occurred in a hefty 24% of 513 Saudi patients placed on isotretinoin for acne. About 42% of those with inflammatory back pain displayed evidence of sacroiliitis on MRI. Moreover, 52% of patients with MRI-proven sacroiliitis fulfilled ASAS criteria for axSpA. In this longitudinal study, the MRI abnormalities and back pain symptoms completely resolved after isotretinoin discontinuation, but it took a long time: up to 9 months.
“When you see these people with inflammatory back pain on isotretinoin, I think it’s important that before you saddle them with a diagnosis that they have axSpA – a diagnosis that will go with them forever – give them time off drug, because this can look like the real thing. It’s something to think about as these pretty young kids come in to see you with back pain: Always ask about their medication history because it could be important,” Ruderman said.
A Successful Biologic Remission Induction-and-Maintenance Strategy
The phase 3b, multicenter C-OPTIMISE study sought to determine the best strategy for avoiding axSpA flares once sustained clinical remission has been achieved with a TNF inhibitor, in this case certolizumab pegol (Cimzia). The first part of the trial involved 736 patients with early axSpA, including 329 with nonradiographic disease. During the 48-week open-label induction period, 43.9% of patients achieved sustained clinical remission at the approved dose of 200 mg every 2 weeks, with similar success rates in radiographic and nonradiographic axSpA.
Those in sustained remission were then randomized double blind to one of three groups: an additional 48 weeks of certolizumab pegol at the full maintenance dose of 200 mg every 2 weeks, reduced maintenance dosing at 200 mg every 4 weeks, or placebo. During this period, 83.7% of the group who continued on full-dose certolizumab remained flare free, as did 79% of those on the reduced maintenance dose. In contrast, only 20.2% of patients in whom the biologic was completely withdrawn remained flare free. The investigators concluded that certolizumab dose reduction is a winning strategy for maintenance of clinical remission, as it reduces costs and limits long-term exposure to immunosuppressive therapy while maintaining clinical benefits.
All Biologics Aren’t Equal When It Comes to Anterior Uveitis Risk
An analysis of Swedish Rheumatology Quality Register data presented at the 2020 EULAR meeting concluded that, among 3,568 patients started on one of four biologics for treatment of spondyloarthritis, the incidence of anterior uveitis was 2.9 per 100 patient-years in those on infliximab (Remicade), 4.0 per 100 patient-years with adalimumab (Humira), 6.8 per 100 patient-years with secukinumab (Cosentyx), and 7.5 per 100 patient-years with etanercept (Enbrel).
“This is important information for us in the clinic. The big question has been, do we see a reduced risk of anterior uveitis with secukinumab, an interleukin-17 inhibitor,” observed RWCS director Arthur Kavanaugh, MD, professor of medicine and director of the Center for Innovative Therapy in the division of rheumatology, allergy, and immunology at the University of California, San Diego.
“When I’ve switched people with uveitis to secukinumab or ixekizumab [Taltz], I do see it come back. So I think it’s important to have these data out there,” Ogdie said.
Certolizumab pegol markedly reduced the incidence of anterior uveitis flares in patients with radiographic and nonradiographic axSpA and a history of recurrent uveitis flares in the ongoing phase 4 C-VIEW study. In the 48 weeks prior to going on certolizumab pegol, the 89 participants included in this analysis had an acute anterior uveitis incidence of 1.5 episodes per patient; during their first 48 weeks on the TNF inhibitor, the rate plunged to 0.2 episodes, representing an 87% reduction.
Secukinumab “Not The Obvious Choice” After Inadequate Response to a TNF Inhibitor
While it might seem logical to turn to an IL-17 inhibitor in patients with an inadequate response to one or more TNF inhibitors, two recently published studies suggest that starting secukinumab is not more effective than trying yet another TNF inhibitor.
A retrospective analysis of Swiss registry data on next-step therapy in 390 axSpA patients who had withdrawn from one or more TNF inhibitors concluded that efficacy at 1 year in the 106 who switched to secukinumab wasn’t significantly different than in the 284 who moved on to another TNF inhibitor.
Similarly, an analysis of 10,583 courses of biologic therapy in 8,050 axSpA patients in five Nordic registries concluded that secukinumab and adalimumab as second-line therapy in patients with inadequate response to an initial TNF inhibitor performed similarly through 1 year of follow-up. However, in patients who’d previously failed to respond to two or three different biologic agents, adalimumab proved superior to the interleukin-17 inhibitor.
“These are two studies that don’t support the intuitive notion of trying a drug with a different mechanism of action when a patient has an inadequate response to a TNF inhibitor. It’s not clear that’s going to make a difference. It doesn’t mean secukinumab can’t work, but it means secukinumab is not the obvious choice,” Ruderman commented.
All three speakers reported financial relationships with numerous pharmaceutical companies.
This article originally appeared on MDedge.com, part of the Medscape Professional Network.
[ad_2]
Source link