[ad_1]
Despite a reputation as potentially double trouble, the Ross procedure of aortic valve replacement provides excellent long-term survival with low rates of reoperation and valve-related complications, according to data from 1988-2018 in the Ross Registry, the world’s largest database of these surgeries.
Among 2444 adult patients followed for a median of 9.2 years (range 0 – 27.4 years), estimated survival was 99.7% at 1 year, 95.4% at 10 years, 79.4% at 20 years, and 75.8% at 25 years.
This is comparable with survival in the age- and sex-matched general population (P = .189), the investigators reported in the March 23 issue of the Journal of the American College of Cardiology.
“The Ross procedure provides excellent survival up to 25 years and if you look at the rate of reintervention and intervention-related morbidity, this is all very low,” senior author Stephan Ensminger, MD, DPhil, University Heart Center Lübeck, Germany, told theheart.org | Medscape Cardiology.
Rates per patient-year for these key outcomes were:
-
Autograft reintervention: 0.69%
-
Right-ventricular outflow tract (RVOT) reintervention: 0.62%
-
Major bleeding: 0.15%
-
Stroke: 0.13%
-
Valve thrombosis: 0.07%
-
Endocarditis: 0.36%
“We were surprised that the RVOT reintervention rate was very low because that’s obviously the Achilles’ heel of the Ross operation because you sometimes get degeneration or regurgitation of the pulmonary homograft,” he said.
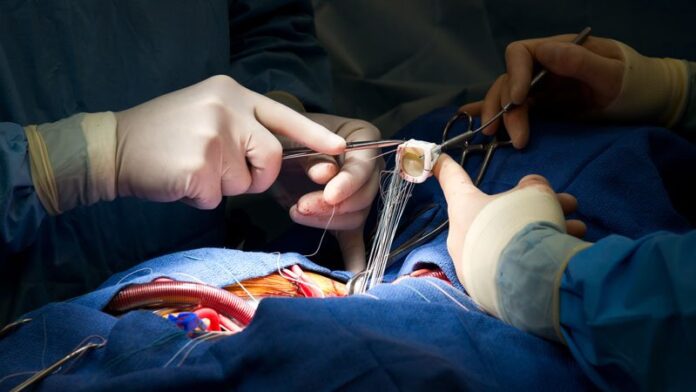
The Ross procedure uses the patient’s own pulmonary valve to replace a diseased aortic valve and then replaces the pulmonary valve with a homograft or xenograft. This is particularly attractive for younger patients requiring aortic valve replacement (AVR) because biological prostheses have limited durability and mechanical valves require lifelong anticoagulation.
The technical demands of the procedure, poor results in the hands of inexperienced operators, and potential for failure of two valves, however, have limited its use.
“The old thing about ‘Now you have two valves at risk’ has turned out to be not nearly as risky as people would think. It doesn’t happen nearly as often and nearly as soon, and there’s some really good data specifically on the state of the pulmonary homograft,” said Paul Stelzer, MD, whose experience with the Ross procedure includes over 550 patients.
For example, a recent study from Australia reported that 99.6% of patients were free from pulmonary allograft reintervention at 15 and 20 years.
“Early on, the naysayers were saying ‘All of those homografts are going to fail within 7 to 12 years’ — well, they were wrong,” Stelzer, a cardiologist at the Icahn School of Medicine at Mount Sinai in New York City who was not involved with the research, told theheart.org | Medscape Cardiology. “The decellularized ones that we’re using considerably now will be even better because they don’t evoke the immune response that may have led to some of the early stenosis that we’ve seen on occasion, but that remains to be seen. It was a pretty good mousetrap before, and to prove we’ve got a better one is going to take a long time and a lot of patients and follow-up.
“That’s the key benefit they’re giving us here — follow-up,” he said. “I think the biggest message is that this can and has been done in centers of excellence for a long time and it has held up. It’s safe and really ends up better long-term, with a very low incidence of reoperation, even though it’s a ‘quote’ two-valve operation.”
Still, current guidelines for valvular heart disease in the United States give the Ross procedure a weak class IIb recommendation, while Ross isn’t even recommended in European guidelines, the authors note. The procedure also struggles for recognition as transcatheter AVR continues its expansion to younger, lower-risk patients.
“In terms of the ever-emerging role of catheter-based therapy, there’s a tendency that this is always compared to surgical valve replacement with biological valves,” he said. “But we think that’s not the whole story, that reconstructive valve procedures also have a role, particularly for younger patients.”
The study included 2444 patients aged 16 years or older at the time of surgery in the Ross Registry. Their mean age was 44 years, three fourths were men, and valve morphology was bicuspid in 63.1% and tricuspid in 20.1%.
The surgeries were performed at 10 European centers, typically by three surgeons (range 2-15). The subcoronary technique was used in 36.5% of cases, root replacement in 19.6%, and root replacement with additional reinforcement in 43.9%.
During follow-up, which was complete in 88%, there were 191 deaths. Early mortality was 1%. Age, diabetes, renal disease, peripheral artery disease, chronic pulmonary disease, and low ejection fraction predicted a shorter time to death.
Similar to the survival time course, the time point of about 13 years after surgery seems crucial to the risk for reoperation and gradually increases from then on, the authors note.
In multivariate analysis, aortic regurgitation (hazard ratio [HR], 1.74) and larger annular diameter (HR, 1.12 per mm) were independent predictors for autograft reintervention, whereas surgical technique was not.
Use of biologic valves rather than homografts was a strong, independent predictor of RVOT reintervention (HR, 8.09), along with younger patient age (HR, 0.97 per year).
Ensminger said he hopes their long-term results, along with another report earlier this month, will elevate guideline recommendations and use of the Ross as a treatment option for nonelderly patients at specialized centers. Efforts are already underway to increase reporting of patient outcomes by expanding the Ross Registry worldwide from its origins in Germany.
“We don’t want to promote or merchandise the Ross procedure,” Ensminger stressed. “We want to optimize patient care on the database to see what has worked and what didn’t work.”
In an accompanying editorial, Ismail El-Hamamsy, MD, PhD, also with Mount Sinai, and colleagues say the study provides further data about the role of the Ross procedure in appropriately selected adults, and that the need for technical expertise combined with proper patient selection underscores the concept of concentration of care in highly experienced comprehensive valve centers to secure optimal outcomes.
“This initiative would require efforts from both societies and the surgical community to train and proctor Ross surgeons, as well as complete transparency in reporting volumes and outcomes from each center with participation in approved national surgical registries,” they write. “While this level of scrutiny may cause some degree of risk aversion, it is ultimately in the best interest of our patients.”
The investigators, editorialists, and Stelzer have disclosed no relevant financial relationships.
J Am Coll Cardiol. Published in March 23, 2021 issue. Abstract, Editorial
Follow Patrice Wendling on Twitter: @pwendl. For more from theheart.org | Medscape Cardiology, join us on Twitter and Facebook.
[ad_2]
Source link